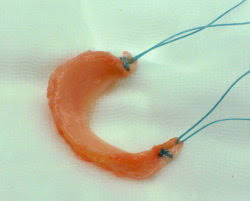
Meniscal allograft transplantation
The meniscal cartilages are two C-shaped wedges of elastic fibrocartilage that sit like rubber washers on the inner (medial) and outer (lateral) sides of each knee, in-between the bones of the femur and the tibia. Their main function is as load sharers, and they increase the contact surface area of the joint thereby reducing peak contact pressures on the articular cartilage that covers the surface of the ends of the bones (the smooth white shiny layer of tissue that makes the bone ends in a joint slippery and low-friction). The meniscal cartilages are often referred to as ‘shock absorbers’ in the knee.
The meniscal cartilages can and often do tear. Meniscal tears in younger patients tend to be from trauma (e.g. twisting on a bent knee). Meniscal tears in older patients tend to be degenerate: as you get older, the menisci tend to lose their elasticity and become weaker, more friable and more likely to tear. About 50% of degenerate meniscal tears occur spontaneously, without any actual trauma.
Meniscal tears can cause pain, swelling, clicking, catching, giving or locking. If a meniscal tear is symptomatic enough to justify intervention, then a knee arthroscopy (keyhole surgery) might be necessary to try and repair the tear, if possible, or else to trim the tear smooth and stable, if the tear is not repairable. Unfortunately, however, only about 25% of meniscal tears are actually repairable, at best.
If a meniscus is torn, then it normally loses at least some of its function. Likewise, if a torn meniscus is trimmed, then there will also be loss of function, and the bigger the tear / the more tissue is trimmed, then the less of a ‘shock absorber’ will then be left in the knee… this leads to an increased rate of wear and tear on the articular cartilage surfaces in that side of the knee joint, which leads to premature degeneration and a very significantly increased risk of arthritis in the knee in the longer-term future.
If a meniscus is removed completely, then the risk of future arthritis in that side of the knee increases by a factor of x15 (i.e. a 1500% increased risk!) by a point 10 years later.
So, if you’ve lost a meniscus in your knee and if you’re beginning to develop progressive symptoms and signs of premature degenerative changes in your knee as a result, then it is possible to replace the missing meniscus by Meniscal Allograft Transplantation.
Is meniscal transplantation new?
No! The first case series of human meniscal allograft transplants was reported by Milchowski, in Germany, way back in 1989. Since then, there have been literally thousands of papers published on the subject, with some outcomes studies reporting outcomes at 26-year follow-up! Unfortunately, however, there are only a small number of centres in UK that specialise in meniscal allograft transplantation and that have extensive experience in this highly specialised procedure.
Mr Ian McDermott has been performing meniscal allograft transplants since 2008, and he is a Hospital Innovations designated ‘Centre of Excellence’ for meniscal transplantation. He has also published widely on the subject of meniscal transplantation and has presented at numerous national and international scientific meetings.
CLICK HERE for further information about Mr Ian McDermott
Can a meniscal transplant get rejected?
The donor meniscal tissue is ‘dead’, with no living cells. The cellular material and cell surface markers within the tissue is bound within a dense matrix of cartilage, and therefore the recipient’s immune system cannot get to it. A donor meniscus does not, therefore, elicit an immune response, and it is referred to as ‘immunoprivileged tissue’, and it does not get rejected. Therefore, anyone can have anyone else’s donor meniscus without the need for tissue typing or the use of steroids or immunosuppressives. One simply has to match left vs right, medial vs lateral and size – and we carefully size-match the donor meniscus to the size of the recipient’s knee but measuring the patient’s knee in advance and then picking an appropriate meniscal allograft from the stock held in registered Tissue Banks (that are fully compliant with all the stringent regulations of the Human Tissue Act, overseen by the Human Tissue Authority).
What about meniscal scaffolds?
A lot of work has gone into trying to develop suitable artificial scaffolds to replace missing meniscal tissue. There are two main types of meniscal scaffold currently available for clinical use:
- the Menaflex / CMI: this is a scaffold made from bovine (cow) collagen that is heat and pressure moulded into a C-shape, and
- the Actifit: this is a polyurethane synthetic scaffold.
Unfortunately, meniscal scaffolds have shown disappointing results, with high rates of the scaffold simply tearing. Also, the tissue that grows into these scaffolds is just scar tissue, not normal proper meniscal tissue. Some studies have show partially positive results, in terms of clinical outcomes (reduction of pain). However, there is nothing better for replacing a missing meniscus other than an actual meniscus, and most meniscal replacement surgeons have given up using scaffolds and only now offer meniscal allograft transplantation as the best and most appropriate treatment option.
What are the outcomes?
Meniscal transplantation has a success rate in the region of about 80 to 85% at 5-year follow-up. However, the probability of a good outcome depends on the overall state of the knee: a knee that has only early / minor wear and tear is likely to do better than a knee where there is more severe and / or more widespread damage.
There is therefore an argument for undertaking meniscal allograft transplantation surgery sooner rather than later – i.e. before it’s ‘too late’. However, meniscal transplantation is a major complex procedure with not-insignificant potential risks, requiring slow and restrictive post-operative rehabilitation, and with no guarantees of a successful outcome. Therefore, we do not recommend people undergoing meniscal transplantation for an asymptomatic knee – i.e. just for ‘prophylactic’ reasons only.
Another important thing to consider is the meaning of the term ‘success’. Meniscal transplantation should very much be considered as just salvage surgery only. It is not ‘restorative’ or ‘regenerative’, as it does not reverse whatever articular cartilage damage might already be present in the joint.
The main indications for meniscal transplantation are to:
- reduce pain,
- improve function,
- reduce the risk of the patient developing fully-blown knee arthritis, and
- the try and delay the time when knee replacement surgery might actually end up being needed
CLICK HERE to read more about what the meaning of ‘success’ is after meniscal transplantation surgery.
Am I too old?
Most surgeons specialising in meniscal transplantation surgery agree that the usual cut-off for this kind of surgery is 50. Some surgeons accept patients up to the age of 55, but this very much depends on the physiological age of the patient and the actual stage of their knee. Unfortunately, meniscal transplantation is not an appropriate option for older patients with full-blown arthritis.
Am I potential candidate?
Before going ahead with meniscal transplantation surgery, it is necessary to undergo a full and detailed assessment, and this needs to include:
- a proper face-to-face assessment in clinic, including a detailed clinical examination
- full up-to-date imaging
- a full, detailed comprehensive discussion with your surgeon about the pros, cons and risks of the surgery, along with a detailed discussion about the rehab and the likely outcomes.
The imaging that is required as part of a full assessment includes:
- a full set of X-rays, with size-markers,
- long-leg weight-bearing alignment X-rays of both lower limbs, and
- a high-quality high-res MRI scan of the joint.
Further information
For further information about meniscal transplantation surgery, please see the following website, which is dedicated entirely to the subject of meniscal transplantation: